Bursitis of the knee
Table of contents
What is bursitis of the knee?
Bursitis refers to the inflammation of a bursa (synovial bursa). This is understood to be a tissue sac that can be thought of as similar to a cushion filled with joint fluid/lubrication (synovial fluid). This cushion supports the sliding of tendons along the bone and cushions the pressure on the knee joint. Inflammation often occurs in the knee joint, but also in the elbow or shoulder, for example.
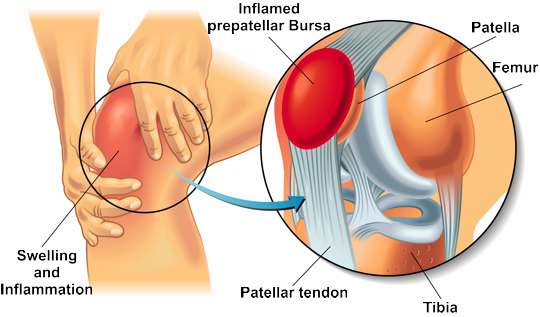
A bursa can become inflamed due to injury, infection, strain or irritation. However, deposited uric acid crystals, as is the case with gout, can also trigger bursitis of the knee. When the bursa is irritated, it fills up with more fluid, thus increasing in volume and requiring more space: it consequently presses on surrounding structures, which can ultimately lead to symptoms. Occupational groups with kneeling activities (e.g. craftsmen) are often affected.
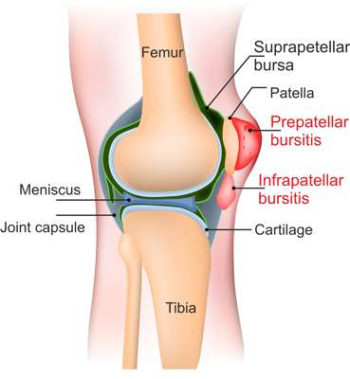
Localisation of bursae in the area of the knee
There are several bursae on the knee where inflammation can occur.
- Suprapatellar bursa: Bursa over the kneecap that communicates with the joint cavity
- Praepatellar bursa: Bursa in front of the kneecap (between kneecap and skin, does not communicate with the joint cavity)
- Infrapatellar bursa: Bursa under the kneecap
There are also other bursae, such as the bursa anserina in the area of the pes anserinus.
Symptoms of bursitis of the knee
At the beginning, bursitis is difficult to notice for those affected. The typical symptoms are slight pain when moving and a rubbing sensation at the site of the inflamed bursa. However, if you continue to exercise, the symptoms can increase. This can be manifested by an overheated and/or reddened knee, a swelling or an effusion. In addition, there may be a feeling of tension and limited mobility of the knee.
Diagnosis of bursitis of the knee
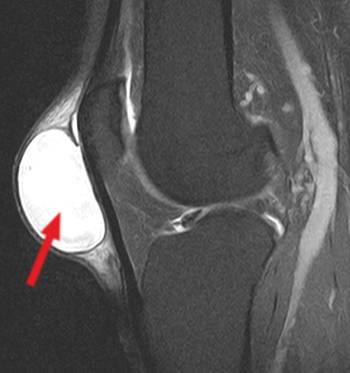
A detailed anamnesis is important for the diagnosis, in which one tries to collect a lot of background information about the course of the disease and the existing symptoms. The affected knee is then examined: a possible bursitis can be determined both by looking at it and by feeling it. In order to exclude other underlying diseases, further examinations such as an ultrasound should be carried out. Ultrasound shows the fluid-filled cavity and a possible thickened wall of the bursa very well. An MRI can also be used to visualise bursitis and exclude other diseases.
Conservative therapy for bursitis of the knee
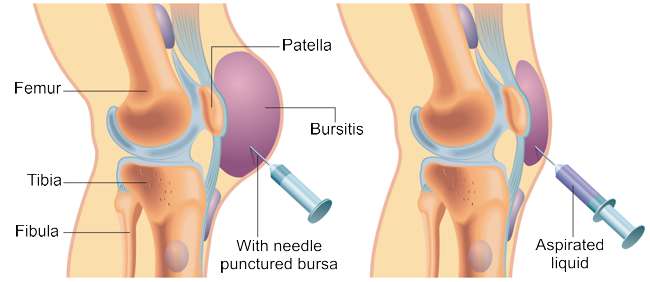
As a rule, bursitis can be treated conservatively, i.e. without surgery. The knee is immobilised (with the help of a splint), rested and cooled. This can be supported by taking pain-relieving and anti-inflammatory medication. If the treatment is effective, the bursitis usually subsides after ten to fourteen days. If the symptoms persist despite the rest and pain medication, cortisone can be injected into the inflamed bursa. The active substance is injected directly into the inside of the bursa and inhibits the inflammation even more. In the case of particularly severe effusions with large swellings, there is the possibility of a puncture: this relieves the pressure and reduces the built-up tension.
Physical therapy such as shock wave treatment and physiotherapy is also supportive. Through targeted training and regular stretching, the strain on the bursa is reduced. As strong muscles protect the joints, they can prevent inflammation in the future.
Surgical therapy of bursitis of the knee
It can happen that the conservative therapy described above does not have a lasting effect and help. If the bursa repeatedly becomes inflamed or the symptoms have persisted for weeks, this is called chronic bursitis. In this case, the bursa can be removed during an operation (bursectomy). In the case of bursitis caused by bacteria, it may also be necessary to remove the bursa surgically: antibiotics are also used here to prevent the bacteria from spreading into the bloodstream.
Aftercare for a bursa removal (bursectomy)
The affected area is less protected without the bursa, but just as mobile as before. After a bursa removal, you can expect to be off work for two to four weeks. However, you should continue to rest the knee for a few weeks afterwards and possibly wear a splint to relieve the strain on the knee. Physiotherapy can also help.