Osteochondritis dissecans (OCD) of the knee
Synonym: Osteochondral lesion
Table of contents
- What is osteochondritis dissecans?
- How does osteochondritis dissecans develop?
- Symptoms of osteochondritis dissecans
- Classification of osteochondritis dissecans
- Diagnosis of osteochondritis dissecans
- Therapy for osteochondritis dissecans
- Conservative therapy
- Surgical therapy
- Ante- and retrograde drilling
- Refixation of the osteochondritis dissecans fragment
- Cell-free matrix transplantation
- Cartilage cell transplantation
- Bone-cartilage transplantation
- Osteochondral allograft transplantation
- Follow-up treatment after surgical therapy for osteochondritis dissecans
What is osteochondritis dissecans?
Osteochondritis dissecans is a disease that leads to cartilage/bone damage (osteochondral lesion) in the joint. This leads to progressive death of the bone underneath the joint cartilage (osteonecrosis). Initially, only the bone is affected and the joint cartilage remains intact. As the disease progresses, cartilage changes also occur until, in the late stages, the cartilage-bone piece is completely detached. The rejected cartilage-bone fragment (also called "joint mouse" or "dissekat") can move freely in the joint and cause damage and blockages of the joint. This subsequently leads to joint wear and tear (osteoarthritis).
Osteochondritis dissecans most commonly occurs in the knee joint (at the medial femoral condyle). However, it can also occur in other joints such as the ankle or hip. It usually affects people who are growing, such as athletic teenagers and young adults. However, it can also affect older people. The course of the disease can vary greatly between young and old.
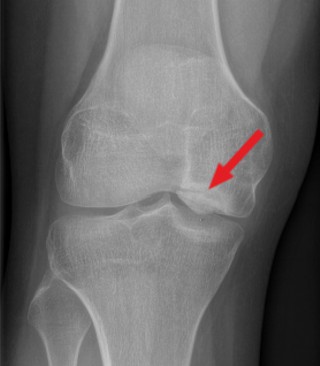
How does osteochondritis dissecans develop?
The causes of osteochondritis dissecans are still not fully understood. In the past, an undersupply of the bone was suspected as a result of a reduced blood supply (ischaemia). In the case of repeated sporting stress in the form of continuous and/or overload, the risk is increased due to possible trauma. This connection is evident in children and adolescents who are active in sports and are still growing. Another influencing factor could be the presence of a leg axis malposition such as bow legs or knock knees. In addition, hereditary components could also play a role.
Symptoms of osteochondritis dissecans
At the beginning of the disease, there are usually no symptoms and the patient is symptom-free. Osteochondritis dissecans is often only discovered by chance in the early stages in the course of an X-ray or MRI performed for other reasons. So it is often an incidental finding. The first symptoms can be unspecific pain in the knee joint, which becomes more pronounced with exertion. If the bone fragment detaches completely at a later stage, more severe complaints may occur. The reason for this is the arthrosis that has developed, which can lead to pain, joint swelling (joint effusion) and overheating. This can also lead to a joint lock. This manifests itself as jamming when stretching and bending the knee in conjunction with sudden pain. Often, the patient's gait changes (e.g. limping). However, the symptoms do not only differ in terms of stage, but can also be pronounced differently depending on age.
Classification of osteochondritis dissecans
Four stages can be distinguished in the course of osteochondritis dissecans (ICRS classification):
- Stage I: stable lesions with intact, softened cartilage
- Stage II: stable lesions with partial (partial) cartilage discontinuity
- Stage III: complete dissection, not yet dislocated
- Stage IV: detached or free dissekat
The more advanced the disease, the more severe the clinical picture is for those affected.
Diagnosis of osteochondritis dissecans
Clinical diagnostics
A detailed conversation (anamnesis) is important in the diagnosis, as it can provide clues to the development of the disease (e.g. regular sporting exertion). However, since osteochondritis dissecans is often asymptomatic in the early phase, the anamnesis can sometimes provide little information. The doctor then proceeds to a physical examination, which provides information about the condition of the knee joint. The doctor examines the knee and moves the joint. Here you can assess, for example, whether the joint is stable or unstable, whether there is any pain from pressure or movement, or whether the patient's movement is restricted.
Diagnostic imaging
The advanced death of the bone (necrosis) can be detected by an X-ray. For the detection of osteochondritis dissecans at an early stage, an MRI (magnetic resonance imaging) is indispensable. An MRI gives precise information about the OCD and possible joint damage. The status of the cartilage and also the size of the bone fragment can be assessed well and thus the current stage can be better estimated. The MRI is an important clue for the prognosis and also for the course of therapy to be assessed.
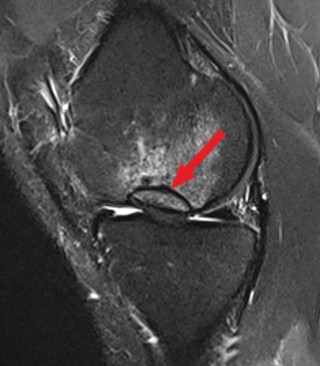
Diseases with similar symptoms (differential diagnoses)
- Ossification disorders: A disorder in the formation of new bone (ossification) can show similar symptoms. This occurs more frequently in childhood and should be differentiated by an X-ray when diagnosing.
- Cartilage defects
- Meniscus tear
- Bone marrow oedema
Therapy for osteochondritis dissecans
The treatment of osteochondritis dissecans is very individual. It depends on the age of the patient, the affected area and the stage or progression of the disease. The aim of treatment is to completely restore the structure and function of the affected joint.
Basically, one can differentiate between conservative and surgical therapy.
In the early stages, osteochondritis dissecans can be treated conservatively. However, as soon as the cartilage-bone fragment has detached, it must either be refixed by surgery or the resulting defect must be treated with different surgical procedures.
Conservative therapy
In stage I of osteochondritis dissecans, conservative therapy is used. Here, the knee joint is consistently spared and relieved over several weeks (e.g. additionally with forearm crutches). This leads to a reduction of the pressure load and allows for improved blood circulation. Above all, sports with stop-and-go movements (such as tennis) or sports with jumping and landing movements should be suspended. During the first weeks of treatment, anti-inflammatory medication can also be taken as an accompanying therapy.
When the pain is gone, everyday activities are possible again without the need for immobilisation. Physiotherapy is also helpful over the next few weeks and months. It serves to improve mobility and build up muscles so that the knee joint is stabilised. Once the findings have been confirmed by an MRI and there is no pain, sport can slowly be resumed.
Surgical therapy
If conservative therapy does not lead to an improvement in the symptoms or if osteochondritis dissecans is already in a more advanced stage, surgical therapy is recommended.
Ante- and retrograde drilling
Drilling is an attempt to heal the fragment into the bone. Tapping can be performed directly from the joint surface through the cartilage surface (antegrade) or from the outside to just below the cartilage/bone boundary (retrograde). The fragment of osteochondritis dissecand must still be stable for drilling (stage I and II), otherwise healing cannot be achieved.
In stage III, advanced cartilage-bone fragments are often found. Healing of the fragment is hardly possible here because the environment around the fragment also changes. In this case, too, only surgical measures can be applied, which are usually carried out by means of arthroscopy. However, due to unfavourable locations or in the case of a large defect, open surgery may also be necessary.
Refixation of the osteochondritis dissecans fragment
Here, the loosened cartilage-bone fragment of osteochondritis dissecans is refixed. For this, the cartilage cover must still be intact. Various choices are available for the refixation, such as bioresorbable materials and metallic screws and pins. If the bone is already severely changed and is not of good quality, it may be necessary to additionally insert autologous bone from another site.
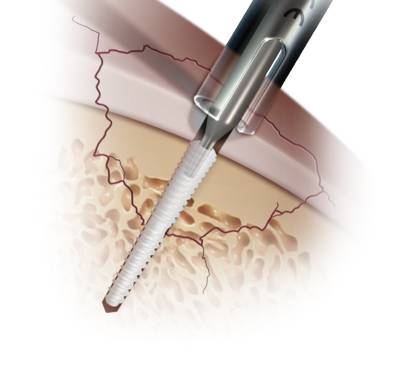
with an absorbable screw (Arthrex)
The second option is to remove the fragment and replace the resulting damage. Since in stage IV of osteochondritis dissecans the cartilage-bone fragment has completely detached from the bone, this is usually the only approach left. To replace the defect after removal of the fragment, the following options are available:
Cell-free matrix transplantation
Synonym: AMIC (Autologous matrix-induced chondrogenesis)
AMIC is a technique that complements microfracturing. First, the bone bed of the osteochondritis dissecans defect is prepared. Then a membrane with a multilayer structure (for bone and cartilage) is inserted into the defect. Stem cells and growth factors from the bone marrow migrate into the defect and attach themselves to the membrane. Over time, this allows a bone and cartilage structure to build up. In the further course, the inserted membrane is resorbed and only the body's own tissue remains.
Cartilage cell transplantation
Synonym: MACT (Matrix-associated autologous chondrocyte transplantation)
Cartilage cell transplantation is particularly suitable for larger osteochondritis dissecans defects. It is carried out in two steps: cartilage cells are taken from an area of the joint that is not under much stress by means of arthroscopy. This is called a biopsy. In the laboratory, the cartilage cells are detached from the surgically removed pieces of cartilage and multiplied there over several weeks. The cartilage cell transplant is then inserted in the second operation about 4-6 weeks after the removal. This procedure is usually done as an open operation, in which the graft is then inserted into the affected area.
If, as in osteochondritis dissecans, the underlying bone is also affected by the damage, this defect can be repaired by filling it with the patient's own bone. This bone graft can be taken from the iliac crest, for example. This is called cartilage cell transplantation with autologous spongiosaplasty. The inserted bone tissue grows together with the surrounding cancellous bone and ossifies. The cancellous bone is the spongy part inside a bone. Consequently, a stable and resilient bone then develops.
Bone-cartilage transplantation
Synonym: OATS (= Osteochondral autologous cartilage-bone transplantation)
In bone-cartilage transplantation, a cartilage-bone cylinder is taken from a low-load area in the joint and inserted into the damaged area of osteochondritis dissecans. The result is a complete and load-bearing cartilage cover. This method is limited, however, as it is not possible to remove an infinite number of cartilage-bone cylinders from the healthy area. Otherwise, damage can occur in the area that is actually free of defects.
Osteochondral allograft transplantation
In osteochondral allograft transplantation, the transplanted tissue for the osteochondritis dissecans defect does not come from the recipient itself, as in the procedure described above. The tissue, also called an allograft, comes from a genetically non-identical donor and is then implanted into the recipient.
Follow-up treatment after surgical therapy for osteochondritis dissecans
The surgical treatment is usually followed by relief of the joint for several weeks. Swelling at the beginning can be reduced by gymnastics and lymph drainage. In order to better assess the effects of the operation, an MRI follow-up is recommended.