Cartilage regeneration, hyaluronic acid, autologous blood therapy
Table of contents
Why does cartilage wear occur?
Articular cartilage is a highly specialised tissue designed to perform its unique mechanical functions. It enables almost frictionless joint movement and distributes pressure evenly throughout the joint due to its high pressure elasticity. The majority of articular cartilage consists of the matrix, a meshwork of various biomolecules (collagens, proteoglycans, hyaluronic acid) and water. Only a very small proportion of the cartilage is made up of cells (approx. 3-5%). These are called cartilage cells or chondrocytes. Their main function is to produce and maintain the cartilage matrix. Since cartilage has no vascular supply, the nutrition of the cartilage cells functions only through the diffusion of nutrients from the synovial fluid. Mature cartilage cells are no longer able to divide. If the cartilage is damaged, there is no supply of cells to rebuild the damaged tissue. For this reason, the joint cartilage hardly has the ability to regenerate itself and cartilage regeneration is difficult.
With increasing age, there is progressive wear and tear of the cartilage (arthrosis). Various factors can accelerate this process, sometimes dramatically (e.g. excessive stress due to overweight or incorrect loading, instability of the knee joint, missing meniscus). The consequence of an injury or joint inflammation can also lead to premature arthrosis.
Treatment strategies for cartilage regeneration
There are various treatment strategies available to us for cartilage regeneration or the reduction of further cartilage wear:
- Change of lifestyle (diet, exercise), weight loss, muscle building, physiotherapy
- Compensation for incorrect loading (shoe inserts, leg axis training, splints, crutches)
- Reduction of the inflammatory process
- Intake or provision of important components of the articular cartilage
- Hyaluronic acid infiltration
- Autologous blood therapy (PRP, ACP)
- Surgical treatment
Cartilage regeneration by hyaluronic acid
Hyaluronic acid is an important endogenous component of the cartilage matrix and the synovial fluid. If the hyaluronic acid is administered into the joint through an injection, it improves the sliding ability of the damaged cartilage due to its special properties. Symptomatically, the pain is relieved. By binding to certain receptors (CD44) on the cell surface of the cartilage cells and synovial cells, hyaluronic acid stimulates the production of cartilage matrix and also has an anti-inflammatory effect. Numerous studies have shown that hyaluronic acid positively influences the growth and matrix production of cultured cartilage cells. Whether a cartilage-building effect can also be expected after infiltration in the arthritic joint is partly discussed differently in the specialist literature. However, there is growing evidence that hyaluronic acid has an arthrosis-modifying effect. This means that, in addition to its symptomatic properties, hyaluronic acid can slow down the progression of cartilage wear. Since hyaluronic acid is a component produced naturally in the body, it is unlikely to have any side effects when used. The effect usually lasts 6 to 12 months. Repeated administration is possible without any problems after the effect has worn off.
Cartilage regeneration by autologous blood therapy (ACP, PRP)
Autologous blood therapy is a procedure that uses the body's own growth factors to stimulate the repair of damaged cartilage tissue in osteoarthritis.
The platelets in the blood contain a large number of different growth factors and proteins that play an important role in the healing and repair of tissue. Many of these growth factors have also been shown to improve the healing of damaged cartilage by stimulating the production of cartilage matrix and blocking factors that damage cartilage. Basic scientific studies have shown that cartilage cells proliferate better in the presence of these growth factors and produce more cartilage-specific matrix (type II collagen and glycosaminoglycans). At the same time, they have an anti-inflammatory effect.
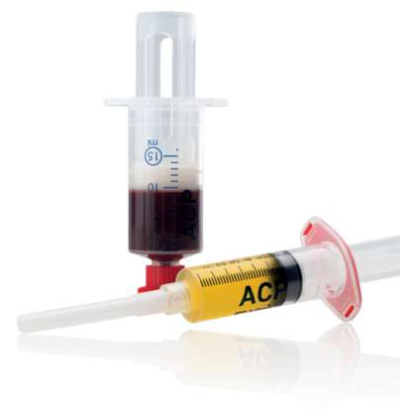
To concentrate the growth factors from the platelets, a small amount of blood is first taken from the patient. The blood is then centrifuged, the blood components separated into different layers and special procedures are used to isolate the layer that is rich in platelets. It is important to remove as many white blood cells (leukocytes) as possible. After preparation, the obtained platelet-enriched blood plasma is injected into the knee joint. For optimal effect, several (3-5) therapy sessions are necessary, each about 1 week apart. After autologous blood therapy, the knee can immediately be loaded normally. The effect of autoblood therapy usually lasts about 12 months. Repeated administration of autoblood therapy is also possible after the effect has worn off.
You can find more information on surgical therapies on the page cartilage defects