Osteoarthritis of the knee (gonarthrosis)
Table of contents
What is knee osteoarthritis?
Osteoarthritis is the wearing away of a joint. Arthrosis in the knee joint is called gonarthrosis (Latin for knee osteoarthritis). The most common cause of knee osteoarthritis is persistent overloading (e.g. due to overweight, malpositions such as bow legs or knock knees, instability after cruciate ligament rupture, (partially) removed meniscus). However, knee osteoarthritis can also be the result of an injury (post-traumatic) or an inflammation of the joint (arthritis).
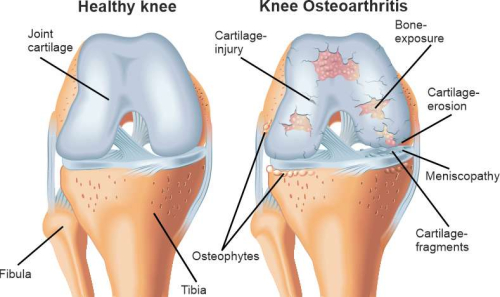
Symptoms of knee osteoarthritis
The symptoms of knee osteoarthritis usually begin gradually. At first, pain may occur more during exertion and later also at rest. A typical symptom is the so-called start-up pain, which occurs mainly in the morning after getting up or after sitting for a longer period of time and improves after a short time. The initial pain can also be accompanied by a certain morning stiffness, which in the advanced stage develops into significant movement restrictions. If a joint effusion occurs (often accompanied by overheating), this is called activated osteoarthritis. This occurs mainly when the patient has put more weight on the knee than usual. On the whole, the maximum load-bearing capacity of the knee joint decreases as the osteoarthritis progresses.
Diagnostics for knee osteoarthritis
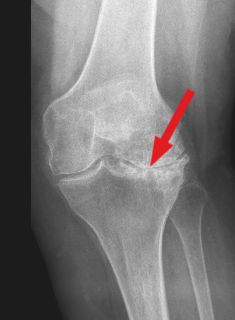
The diagnosis is made through a precise assessment of the symptoms, a thorough clinical examination and imaging procedures such as an X-ray examination. X-rays show signs of osteoarthritis such as a narrowing of the joint space and bone compression very well. Magnetic resonance imaging (MRI) is usually not necessary. However, an MRI can be helpful in distinguishing isolated cartilage damage from incipient osteoarthritis.
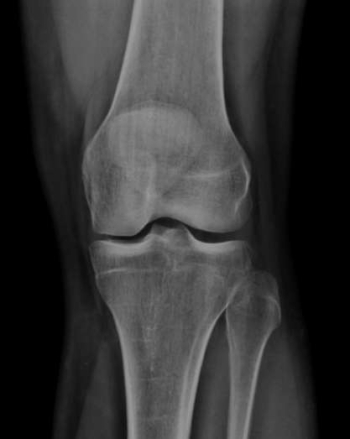
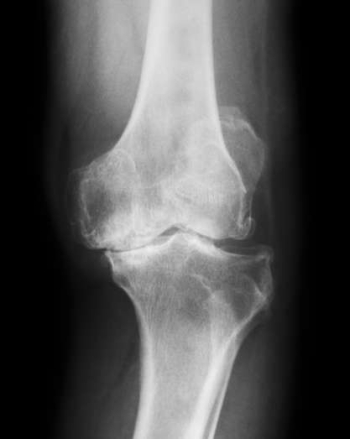
Forms of knee osteoarthritis
Both the cartilage between the femur and the tibia (tibiofemoral joint) and between the femur and the kneecap (patellofemoral joint) can be affected. Depending on which section is involved, the symptoms occur in different locations.
Tibiofemoral osteoarthritis
The joint between the femur and the tibia can be divided into an inner and an outer compartment. The leg axis is the axis through which most weight is transferred to the tibia, feet and ultimately the ground and should pass through the centre of the knee joint so that ideally both knee joint compartments are equally loaded. If, however, the joint axis shifts outwards or inwards in relation to the centre of the joint, this results in knock-kneed or bow-leg malalignments with corresponding incorrect loading. In technical jargon, this is called a valgus or varus deformity. For very few people, the axis runs perfectly through the middle of the knee joint. However, if the deviation is too strong, it can lead to osteoarthritis.
Varus gonarthrosis (bow-leg malalignment)
The knees diverge in an O-shape. The leg axis lies further inwards than the centre of the knee joint and runs through the inner compartment of the tibiofemoral joint. Accordingly, the body weight is now more likely to be transferred to the tibia via the inner compartment, which is why there is also more rapid wear of the medial meniscus and the internal cartilage. Radiographically, one notices a narrowing of the joint space of the inner compartment of the joint. For the patient, this means an increased perception of pain on the inside of the knee.
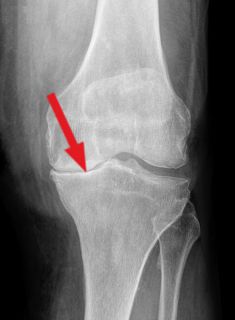
Valgus gonarthrosis (X-leg malalignment)
The knees point inwards in an X-shape. The leg axis deviates outwards from the centre of the knee joint and runs through the outer compartment of the tibiofemoral joint. This leads to overloading of the outer joint compartment. This manifests itself in wear of the outer meniscus and the outer articular cartilage and can be detected in X-rays by a narrowing of the outer joint space. The patient will therefore also notice the pain more on the outside.
Patellofemoral osteoarthritis
The kneecap (patella) forms a joint with the thigh bone (femur) (patellofemoral joint). It is covered with cartilage on its back and lies in a sliding groove of the femur, which is also covered with cartilage. The patella can therefore move smoothly up and down in the sliding bearing of the femur when the knee joint is extended or bent. If the pressure of the patella on the femur is now increased (e.g. by kneeling down, walking downhill, going down stairs), this leads to increased cartilage wear and ultimately to osteoarthritis behind the kneecap. Very often, due to deformities (patellar dysplasia, trochlear dysplasia), the patella does not lie perfectly in the gliding groove. As a result, pressure points develop that promote cartilage damage when the knee joint is moved. Patellofemoral osteoarthritis is usually noticeable through pain behind the kneecap.
Treatment of knee osteoarthritis
Treatment depends mainly on the cause and how advanced the knee osteoarthritis is. If it is possible, the cause of the osteoarthritis should always be eliminated. If, for example, a malalignment is found as the cause and only part of the joint is affected (inner or outer side), a correction of the malalignment (osteotomy) can bring about an improvement in the symptoms and prevent or slow down further progression of the osteoarthritis.
In the early stages of knee osteoarthritis, conservative therapy (physiotherapy, movement exercises, muscle building, pain therapy with medication) is the first step. The aim of conservative therapy is to reduce pain and improve the function of the knee joint. In addition, injections into the knee joint (infiltrations) with hyaluronic acid or the patient's own blood (PRP, ACP) can lead to an improvement in the symptoms.
Physiotherapy for knee osteoarthritis
With numerous movement exercises and targeted muscle building, physiotherapy is a cornerstone of osteoarthritis treatment. The effectiveness of physiotherapy with the clinical endpoints "freedom from complaints" and "mobility" has been proven in numerous studies. In the case of leg axis malalignment that does not require immediate surgery, physiotherapy can even achieve a slight leg axis correction through targeted training. A well-conducted physiotherapy can therefore strongly influence the course of the disease, alleviate symptoms and delay the date for a potential knee surgery.
Hyaluronic acid infiltrations - "cartilage regeneration"
Hyaluronic acid is an important component of joint cartilage and synovial fluid. Studies have shown that there is a lower concentration of hyaluronic acid in worn (osteoarthritic) joints than in healthy joints.
Infiltrations of hyaluronic acid into the joint lead to the cartilage being able to store more hyaluronic acid again and the joint fluid being able to better perform its function as a joint lubricant. In addition, hyaluronic acid has an anti-inflammatory effect and thus blocks enzymes that contribute to cartilage destruction.
Hyaluronic acid infiltrations are administered either 5 times in a row at weekly intervals or once (highly cross-linked hyaluronic acid). The effect usually lasts 6-12 months.
In cases of severe pain, irritation and knee joint effusions, as can occur in activated osteoarthritis, infiltrations with cortisone are used. Cortisone has a strong anti-inflammatory and analgesic effect. However, due to numerous side effects, long-term therapy with cortisone is not recommended.
Knee replacement
In the case of advanced osteoarthritis and lack of success of other treatment methods, the implantation of an artificial joint replacement (knee prosthesis) makes sense. During the implantation of a knee prosthesis, the destroyed parts of the joint are removed and an artificial joint is inserted. A distinction is made between a replacement of the entire knee joint (total endoprosthesis) and a partial joint replacement (hemiarthroplasty or patellofemoral replacement). A partial joint replacement is only possible under certain conditions and is used much less frequently than a total endoprosthesis. The average lifespan of a knee prosthesis depends on the patient's age, activity, weight and bone quality and is currently around 15-20 years.
You can find more information on the topic of artificial knee joints in the chapter: Knee replacement