Knee pain: forms and causes
Table of contents
Structure of the knee joint
The knee joint is the largest joint in the human body and is characterised by a complicated anatomical structure. Three bony joint bodies meet in the knee: the thigh bone (femur), the shin bone (tibia) and the kneecap (patella). The bones form two joints between them: Tibiofemoral joint (between femur and tibia) and Patellofemoral joint (between patella and femur). One therefore also speaks of a compound joint.
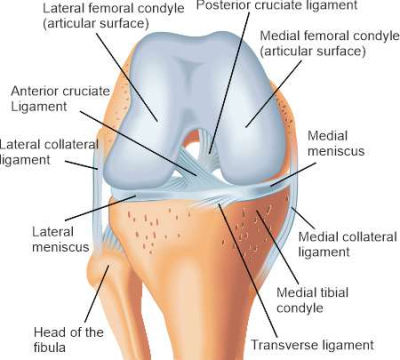
The kneecap lies in a sliding groove of the femur and serves as an intermediate attachment of the tendon of the large knee extensor (Musculus quadriceps femoris), which ultimately radiates into the tibial head at the front. This increases the distance between the muscle and the centre of rotation of the axis of movement of the knee joint and results in greater force development - as with a lever. It also gives the knee protection from external shocks. The joint surfaces are all covered with abundant cartilage between each other, which allows the joint partners to slide smoothly against each other. Since the knee joint has to withstand the heavy loads of the body weight, the menisci are inserted as an additional buffer at the place of greatest mechanical stress - namely between the femur and the tibia (tibiofemoral joint). When the cartilage or menisci wear out (gonarthrosis), the cushioning effect is lost when the knee joint moves and the bones rub against each other painfully. The joint is stabilised by numerous ligaments and muscles, as well as a connective tissue joint capsule. Due to the complex structure and the great stresses to which the knee is exposed throughout its life, the causes of knee pain can be very diverse.
Forms of knee pain
In principle, a distinction is made between acute knee pain and chronic pain, whereby acute knee complaints are usually of post-traumatic origin - i.e. they occur after an accident - and are easy to ascertain from the doctor's consultation.
Pain manifests itself very differently in people and is often also perceived differently. Therefore, it is important to classify knee pain in a uniform way.
- Start-up pain
Occurs at the beginning of a movement (e.g. getting out of bed in the morning, getting up after sitting for a long time, walking after standing for a long time) and is typical of osteoarthritis. Often, start-up pain can be accompanied by some morning stiffness, but this usually resolves within half an hour. - Strain pain
Describes a pain that only occurs with physical exertion or mechanical strain. The pain disappears again at rest. Characteristic causes are mainly traumatic injuries, such as after accidents or in sports injuries, but in the case of knee joint inflammation and osteoarthritis, the strain can of course also be painful. - Pain at rest
Can already occur during physical inactivity (e.g. when lying or sitting) and are more indicative of inflammatory diseases of the joints such as chronic polyarthritis (= rheumatism) or infection. It can also happen that after overloading an arthritic knee joint or in the case of severe cartilage damage, the pain from exertion changes into pain at rest. From an orthopaedic point of view, pain at rest is therefore an important criterion to get an idea of the severity of the underlying disease of the affected joint and often decisive for the decision of the further therapy procedure (conservative or surgical, joint preservation or joint replacement).
However, in order to be able to make a tentative diagnosis, additional information is required. Pain quality (e.g. burning, stabbing, pulling, pressing, ...), localisation, duration, radiation and any accompanying symptoms are taken from the medical consultation (anamnesis) and point to the correct cause. In the case of acute knee pain, for example after an accident, information about the exact accident is of great importance. In the case of chronic pain, it is necessary to determine when and in which situations the pain increases or decreases. This can depend on the time of day or on the movement sequence during which the knee pain increases in intensity. The decision on further diagnostic procedures, such as imaging by MRI or X-ray, is always ultimately made after the clinical physical examination.
Accompanying symptoms of knee pain
The following symptoms may accompany knee pain.
- Protective posture
The knee is not only the largest joint in the human body, but is also characterised by a complex capsular ligament apparatus that enables people to distribute the large mechanical loads of their body weight evenly and thus ensure locomotion. Particularly in the case of unilateral knee pain, a protective posture is often adopted in which the weight is shifted from the painful knee to the other. As a result, the non-painful knee is subjected to greater strain, which quickly leads to wear and tear on the "healthy" knee. - Radiation into the hip, upper or lower leg.
Very often, knee pain occurs as a secondary cause as a result of hip joint disease. The pain is then projected from the hip via the nerve pathways to the thigh and knee. Via the same mechanism, back problems (e.g. herniated disc) can also cause pain over the entire leg. - Movement restriction
- Tension or hardening of the muscles
- Redness, warmth
- Swelling
- Crackle/Gnash

Possible causes of knee pain
There are numerous knee joint diseases that are associated with pain. As mentioned above, the localisation and type of pain can already indicate possible causes.
Front (anterior) knee pain
- Retropatellar osteoarthritis (cartilage wear behind the kneecap)
- Fracture (bone fracture, e.g. of the kneecap)
- Patellofemoral cartilage defects (cartilage damage between the patella and the sliding bearing of the femur).
Possible with:
- Luxation of the patella
- Lateral hypercompression syndrome (outward displacement of the patella with increased pressure on the thigh bone)
- Post-traumatic
- Patellar tendinopathy (Jumper's knee)
- Patellofemoral pain syndrome (PFS)
Especially for young people - Patellar dysplasia/trochlead dysplasia (differently shaped patella/sliding groove)
- Osgood-Schlatter disease (Rugby Knee)
Painful irritation of the attachment point of the patellar tendon at the head of the tibia, which often occurs in young athletically active patients due to training. Because the growth plates have not yet fully hardened, prolonged stress due to too intensive training can lead to inflammation of these areas on the anterior tibia. The typical age of patients with Osgood-Schlatter disease is 9 - 14 years.
As you can see, pain in the front of the knee is a clear indication of a problem with the kneecap. If the knee pain also occurs when walking downhill (hiking, going down stairs), this would be another indication of a disease or injury involving the patella.
Outer (lateral) knee pain
- Injury to the outer collateral ligament
- Injury to the outer meniscus
- Cartilage damage in the outer joint compartment (tibiofemoral lateral)
- Fracture (bone fracture, e.g. of the external tibial condyle)
- Valgus gonarthrosis
X-leg malalignment with an accompanying excessive load on the external joint space of the tibiofemoral joint - Coxarthrosis (hip osteoarthritis)
Hip pain in the context of hip osteoarthritis very often radiates to the outside of the knee. One should therefore always think of an underlying hip joint disease. - Disc prolapse (herniated disc)
In the case of a slipped disc, the pain can also radiate from the back along the nerve pathways to the knee. - Iliotibial band syndrome (runner's knee)
Inner (medial) knee pain
- Injury of the inner collateral ligament
- Injury of the inner meniscus
- Cartilage damage in the inner joint compartment (tibiofemoral medial)
- Fracture (bone fracture, e.g. of the inner tibial condyle)
- Varus gonartrosihs
O-leg malalignment with an established excessive load on the inner joint space of the tibiofemoral joint - Buckled flat foot with associated overloading of the knee
Knee pain in the hollow of the knee
- Baker's cyst
A Baker's cyst that is too large can compress nerves behind it and thus cause pain in the back of the knee, but also numbness. - Injury in the inner or outer posterior horn of the meniscus
- Osteoarthritis
Postoperative knee pain
After an operation, depending on the type of surgical procedure (arthroscopy, open surgery), pain may occur in or around the knee. This is related to the wound area and the absence of joint fluid (e.g. after an arthroscopy). Often the knee also swells postoperatively. This type of knee pain does not usually require treatment (except with painkillers prescribed by your doctor) and should subside after some time. If the symptoms persist or worsen (especially if redness, fever, chills appear), a medical examination should be carried out in any case. If there is pain in the calf, a leg vein thrombosis should also be ruled out.
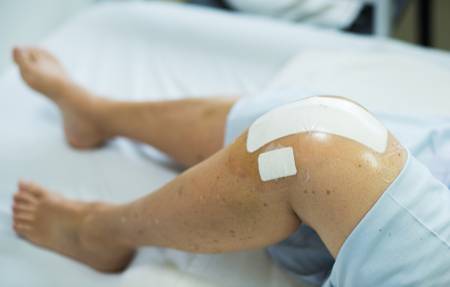
Other causes of knee pain
Knee pain cannot always be localised or described exactly. For example, in the case of bursitis (= inflammation of the bursa), the pain can be felt in the entire knee area.
In more complicated cases, other diagnostic methods should be used. If, for example, there is a suspicion of an underlying rheumatic inflammatory disease with involvement of the knee joint, then a laboratory blood test with a check of the inflammatory parameters/rheumatism factors should be carried out in any case, since untreated rheumatoid arthritis can lead to irreversible damage to the joint. The same applies to any suspected infection in the knee joint (infectious gonarthritis). If there is an effusion in the knee joint, the fluid can be aspirated (punctured) and sent to the laboratory for further examination.
When should you see a doctor for knee pain?
A medical assessment should be carried out in any case if the knee pain is:
- Persistent and/or massive and thus have limitations in coping with everyday life
- Recurrent (occurring again and again)
- Sudden and very strong onset (for example after an accident)
- Accompanied by redness, warmth, swelling or other signs of inflammation such as fever
In addition, accompanying symptoms such as cracking/crunching, but also instability of the knee joint require a medical assessment. Since long-term damage can often be avoided through timely treatment, it is advisable to always consult a doctor in case of knee pain.